How we save lives / Epidemic prevention / Epidemic-Ready Primary Health Care
Epidemic-Ready Primary Health Care (ERPHC)
Making sure that every primary health care facility is equipped to prevent, detect and respond to outbreaks while maintaining essential services
Right: Participants in “Law & Health Security: Strengthening Nigeria’s Legal Preparedness”. Credit – Resolve to Save Lives

Challenge
Primary care facilities are our first line of defense against infectious disease outbreaks, but they’re rarely set up for success in preventing epidemics.
Solution
We partner with facilities to get them “Epidemic-Ready” — equipped to spot and report cases early, manage them safely, and handle surges without disrupting essential care.
Impact
Epidemic-Ready facilities detect and respond to outbreaks faster, experience fewer health care worker infections, and save more lives by preventing epidemics before they start.
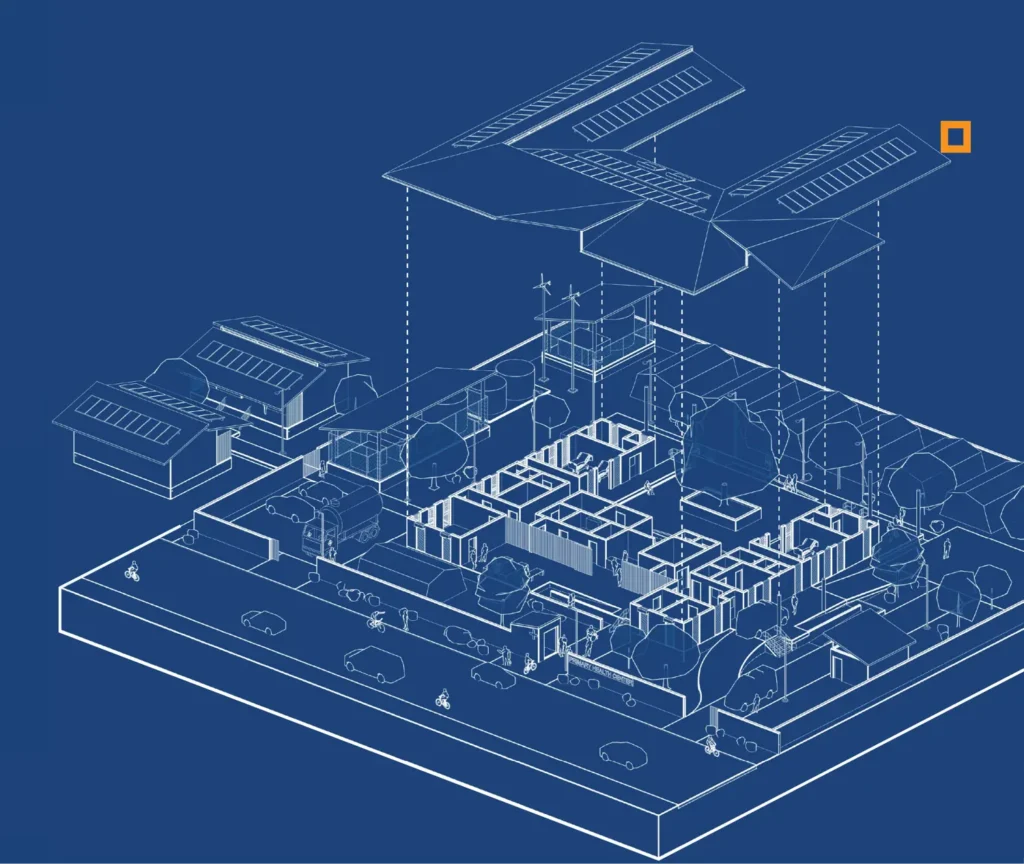
What is Epidemic-Ready Primary Health Care?
Epidemic-Ready Primary Health Care (ERPHC) helps strengthen local health systems so they can prevent, detect, and respond to outbreaks while continuing to provide everyday health services to their communities.
ERPHC ensures primary health care systems can quickly identify and notify cases, manage them safely and handle increased patient volume while continuing to maintain essential services.
To achieve this, ERPHC enables frontline health care workers to:
Connect
Build deep, trusting relationships with the communities they serve.
Detect
Identify and promptly report suspected disease cases.
Protect
Apply the correct infection prevention and control measures.
Treat
Continue delivering routine services during outbreaks.
Highlights
How ERPHC works
Resolve to Save Lives partnered with 1,000 primary health care facilities in Ethiopia, Nigeria, Sierra Leone and Uganda to pilot ERPHC. Key interventions included:
-
Integrating key areas such as disease surveillance, infection prevention and control and case management.
-
Simplifying technical resources for frontline workers so they’re easier to understand and use.
-
Building knowledge, skills and confidence of health care workers through regular mentorship.
-
Strengthening public health emergency management to keep essential health services running during crises.
-
Providing tailored, just-in-time training for health care workers during times of heightened risk.
-
Regularly assessing capacities and using data to plan and improve performance.
-
Improving communication and coordination between primary health facilities and public health authorities.
-
Strengthening national infection prevention and control programs and advocating for increased domestic financing.
From “Epidemic-Ready” to “Emergency-Ready”
Based on our learning from implementing ERPHC, we partnered with WHO to develop the Emergency-Ready Primary Health Care framework—an all-hazards approach to strengthening preparedness and resilience at the frontline. The framework translates global guidance into a practical, operational model for countries, defining the core capacities needed and how they can be integrated into systems.

Measuring our impact
Using a tool we developed to identify strengths and areas for improvement, each health facility is given an “ERPHC score” that measures its overall capacities in three essential areas. In less than a year, all participating facilities reported improvement in all three:
- ERPHC scores: including gains in hand hygiene, infection prevention and control behaviors and clinical suspicion, which is a major bottleneck in many outbreaks.
- Case detection and reporting: with many participating facilities now meeting the 7-1-7 target.
- Surveillance: leading to an increase in quantity and quality of alerts from facilities to national reporting systems.
To understand how ERPHC scores correspond to health care worker behaviors during a crisis, we use patient simulation exercises, in which an actor displaying real symptoms arrives at a health facility during a scheduled visit from an ERPHC mentor. These exercises help identify gaps between readiness capacities and real-world performance.
We were scared to open during COVID. We didn’t think we could manage, but with support we treated hundreds of patients as one of the only clinics in the district that had oxygen. Then, not long after COVID, Ebola came. Again, the staff were scared, and we weren’t sure we could stay open. But the mentors came and trained us, helped us with protocols for triage and set up an isolation room… We felt prepared, we felt ready, we no longer needed to run.
Sister Hilda, Head Nurse at Wanda Health Centre, an ERPHC partnering facility in Uganda